 Olivia Twenty Dahl (1955-1962) Olivia Twenty Dahl (1955-1962) In 1962, a seven-year-old girl named Olivia brought home a note from school warning about an outbreak of measles in her class. Soon Olivia too was running a mild fever and covered with red spots. Over the next few days the disease ran its expected course, and her parents weren’t particularly worried. To while away the time, her doting father amused her by telling her stories, teaching her to play chess (at which she promptly beat him), and showing her how to make figures from pipe-cleaners. Then one morning, just as Olivia appeared to be nearly recovered, her father noticed that she had suddenly become feverish and unresponsive, stirring only to moan about a headache. Within just a few hours she was dead from measles encephalitis, a serious complication for which to this day the best medicine can offer is supportive care. Olivia’s father, Roald Dahl, author of such children’s classics as Charlie and the Chocolate Factory and James and the Giant Peach, was “limp with despair.” Dahl was a “do-something” sort of person. When his infant son had suffered brain damage in an accident a couple of years earlier, he had actually set about to design a valve to prevent blockage of the shunt that drained fluid from the brain - and succeeded. He was no biomedical engineer, but when the need arose, he assembled a small team and acquired sufficient expertise to meet the challenge. Now, with Olivia’s life hanging in the balance, there was nothing he could do. He was haunted by his sense of helplessness, compounded after her death by inchoate feelings of guilt that he had somehow let his daughter down. And yet, what could he have done? Twenty-six years later, hoping to extract some shred of meaning from Olivia’s death by sparing others a similar fate, he wrote, “[T]here is today something that parents can do to make sure that this sort of tragedy does not happen to a child of theirs. They can insist that their child is immunised against measles. I was unable to do that for Olivia in 1962 because in those days a reliable measles vaccine had not been discovered. Today a good and safe vaccine is available to every family and all you have to do is to ask your doctor to administer it.” * * * * * * * * * * Measles. The very word sounds slightly risible. Like “Measles the Clown,” perhaps. Or trifling. Like “just some measly childhood disease.” 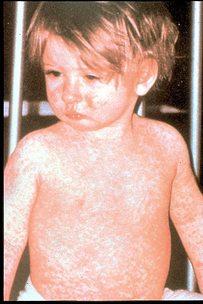 (courtesy of the Centers for Disease Control and Prevention) (courtesy of the Centers for Disease Control and Prevention) But measles is no joke. It is highly contagious and can be spread by an infected person up to four days before before the telltale rash emerges, via tiny airborne droplets produced by sneezing or coughing that remain suspended in the air for two or more hours, even if the infected person is no longer in the room. In many victims the disease runs a benign course, but one in ten are hospitalized, some of whom suffer serious complications including pneumonia and encephalitis. Around 1 or 2 in every 1,000 victims die. Prior to the development of a vaccine, nearly everyone in the US contracted the measles by age 15 - that is, an estimated 3 to 4 million cases/year - so the mortality rate of .1-.2% added up to many thousands of victims per year, mostly children. Measles still causes more vaccine-preventable deaths worldwide than any other infectious disease. A live measles vaccine was first licensed in 1963, just a year after the tragic death of Olivia Dahl, and was superseded by an improved version in 1968. In the twenty years following its introduction in the US, an estimated 52 million cases of measles were prevented, with corresponding dramatic reductions in measles-related complications and death. In the year 2000, measles as an endemic disease was officially “eliminated” from the US; the only reported occurrences of measles were occasional cases introduced from abroad. Truly a public health triumph. Though measles persists globally, most notably in developing countries, aggressive vaccination campaigns have resulted in a precipitous drop in mortality from measles complications worldwide, with a 75% decrease between 2000 and 2013. We now have a measles vaccine that is 97% effective after a single dose and close to 100% effective after a booster dose, which has been recommended since 1985. (Note: People born between 1957 and 1984 should review their immunization status with their doctor, especially if they are planning foreign travel.) To reduce the pain of multiple injections, the vaccine is almost always administered in combination with vaccines for mumps and rubella (MMR) - the first at 12-15 months (earlier if travel abroad is planned), the second at 4-6 years. The rate of serious or life-threatening complications following MMR vaccination is vanishingly small. Although there is NO evidence whatsoever to support a link between MMR vaccine and autism, and although that claim has long since been proved a hoax, the preservative thimerosal (the supposed villain) is no longer used in any vaccine administered to children. As a result, “do-something” parents like Roald Dahl actually have something they can do to ensure that Olivia's fate is not shared by their own child: "They can insist that their child is immunised against measles.” * * * * * * * * * * End of story? Sadly, no. For a disease that’s supposedly been eliminated, measles seems to crop up in the news surprisingly often. After reaching a low of 37 cases in 2004, we now spike record highs every few years, peaking at 667 cases in 2014. A 2013 outbreak occurred at a megachurch in Texas whose pastor had preached from the pulpit against vaccination. In 2015, nearly 200 cases in 24 states were traced to exposure after visits to Disneyland in California. Currently making headlines is an outbreak in Minneapolis, starting in the Somali-American community (fueled by anti-vaccine advocates from outside the community who prey on worries about autism, a malicious genie that refuses to go back in the bottle) and fanning out into the surrounding population through contact in the public schools.
These outbreaks are all shots over the bow. Because international travel is so commonplace, the occasional introduction of measles from abroad is inevitable so long as the disease remains a global scourge. Even more troubling is the occasional case in which no known link to international travel can be found, raising the specter that the disease might once again become endemic. But regardless of the source of any given case of measles, what happens next - whether that single case is self-contained, leads to isolated regional outbreaks, or triggers a full-blown epidemic - depends on how many susceptible individuals are subsequently exposed. Who are these susceptible individuals? As noted above, a handful remain vulnerable even though they have been vaccinated - especially if they have not received a booster dose. In addition, some people are ineligible to be vaccinated because they are very young or very old, because their immune systems are compromised due to illness, because they are pregnant, or in very rare instances because they are allergic to some component of the vaccine. The rest of the susceptible population consists of individuals - mostly children - who though medically eligible have not been vaccinated - and herein lies the problem. Because measles is so highly contagious, vaccination coverage needs to be reach around 95% to maintain “herd immunity” and prevent further spread once a case is introduced. Doing the math, almost everyone who is medically eligible must be vaccinated to prevent the spread of measles, on a regional level or potentially on a much larger scale. Epidemiological studies of measles victims have repeatedly shown that most had not been vaccinated, and of these, the majority had been exempted for non-medical reasons relating religious or philosophical beliefs, or to the systematic spread of discredited data about the health risks of vaccinating (negligible) vs not vaccinating (potentially lethal). Consequently, vaccination rates continue to fall short of the 95% threshold in communities in many areas of the country. The underlying cause of the societal breakdown that could lead to such a situation is difficult to pinpoint. Parents may be uninformed about the importance of completing immunization schedules in a timely manner or persuaded that they cannot trust scientific findings or governmental protections. They may believe their responsibility to their own children takes precedence over the social contract stipulating that we all accept small risks to avoid much larger risks to society as a whole, without understanding the risks to which they subject their own children by leaving them defenseless against measles. Government agencies in turn may succumb to pressure to issue non-medical "personal belief" exemptions or be reluctant to enforce existing vaccination requirements. People with far more expertise than I can claim have yet to figure out where to intervene in this chain and how hearts and minds can be changed. Part of the problem, of course, is that thanks to the very success of immunization campaigns, many Americans have lived their entire lives without having witnessed the ravages of a major epidemic. Let us hope an answer can be found that doesn't require a reintroduction of some of the terrifying communicable diseases medical science has conquered. How fortunate we are to live in a time and place where children like Olivia no longer need to die as their parents stand by helplessly. How sad that some will anyway, and that there is no immediate end in sight to this trend.
0 Comments
Pertussis or whooping cough (named for the characteristic though occasionally absent “whoop” at the end of a coughing episode) is a potentially serious disease at all ages but particularly in very young infants. It starts out deceptively resembling a cold, with a runny or stuffy nose, sneezing, and a mild cough. Over the next week or two, the cough becomes increasingly severe, with violent repeated coughing, gasping for breath after a coughing fit, difficulty eating and drinking, sometimes progressing to dehydration and exhaustion as well as pneumonia. About half the babies afflicted with pertussis will spend time in the hospital. Some will die.
From 1926-30, more than 36,000 deaths from pertussis were recorded in the US. Then, in the early 1940s, an effective vaccine was developed. Although its side effect profile was not completely benign (mostly mild but in rare cases, seizures), it was a relatively safe procedure compared to the risks of pertussis and by 1948 had led to a dramatic decrease in whooping cough cases and deaths. Indeed, some even dared to hope the disease could be eradicated. (So far, even to this day, only one human disease, smallpox, has been completely eradicated, along with a handful of diseases that were once the scourge of livestock.) In the 1970s, just as the disease was reaching a historically low ebb, controversies about the safety of the Diphtheria-Pertussis-Tetanus (DPT) immunization erupted around the world. Documentaries and newspaper reports purporting to demonstrate neurological damage alarmed the public, followed by an even more inflammatory 1982 film entitled Vaccination Roulette, which claimed the immunization could cause permanent brain damage. Victim advocacy groups sprang up, lawsuits against manufacturers were filed, vaccine prices rose, and some companies even discontinued manufacturing the vaccine. Research confirming the safety of the DPT immunization and a strong counter-response especially in the US somewhat calmed but could not fully quell the furor. Immunization rates went down. Sound familiar? This predated the media storm provoked by the fraudulent research of Dr. Andrew Wakefield demonizing the Measles-Mumps-Rubella immunization and its supposed connection with autism, and perhaps even provided a template for that campaign. For better and for worse, these concerns led to the development of a new pertussis vaccine, introduced in 1998, which causes fewer side effects and is better tolerated but also wears off more quickly and may be less effective. Pertussis, once thought to be consigned to the junk heap of history, has now come roaring back, with a measurable increase in baseline levels of the disease and epidemics every few years during which morbidity and mortality spike. It is far more common that other vaccine-preventable diseases such as measles and rubella. The reasons for this resurgence have yet to be fully explained. In part it may simply be an artefact of improved surveillance in adults - in whom, make no mistake, pertussis can also lead to serious illness. Genetic changes in the bacterium and the reformulation of the vaccine may also have contributed. There can be little doubt that reduced uptake of the vaccine, further fueled by the more general suspicion of vaccination that now prevails in the US, is also a factor. Numerous studies have demonstrated a negative correlation of pertussis vaccination rates with both morbidity and mortality. * * * * * * * * * * * * * * * The biggest chink in our armor has always been the youngest sector of the population, infants who have not yet started or have only partly completed the immunization process. They are at once the most vulnerable to serious complications and the least protected from exposure. As Dr. Benjamin Spock warned in 1946 - in stark contrast to his generally reassuring tone - pertussis is “a disease to avoid like the plague if you have a baby in the household.” Those words remain as true today as when first he uttered them. The vast majority of pertussis deaths occur in infants aged 3 months and under. The immunization sequence starts at age 2 months; after a series of boosters, the child is considered fully immunized at age 15-18 months when the fourth shot is administered. Until then, babies and especially newborns are desperately in need of societal protection. How best to provide that protection, however, is a topic that continues to evolve. Initially the Center for Disease Control’s recommendations focused on “cocooning,” encircling each newborn with an impenetrable shield by avoiding exposure to anyone who might possibly have the disease. Among people with pertussis, even those who may not know they have it, the attack rates among “susceptible household contacts” (that is to say, mostly babies) are as high as 80%, so the goal was to ensure that parents, siblings, and caregivers were vaccinated. Beyond that, or failing that, babies were dependent on herd immunity - that is, minimizing the spread of the disease by maintaining a vaccination rate high enough to reduce the likelihood of exposure to an active case. The percentage of vaccinated individuals needed to provide herd immunity varies from disease to disease but for pertussis is well above 90%. Because this approach did not produce fully satisfactory results, the CDC in 2013 modified and expanded its strategy: Instead of focusing solely on cocooning, it first and foremost emphasized vaccination of all pregnant women irrespective of previous history of vaccination, ideally in the last trimester of every pregnancy, in order to confer passive immunity on the infant until s/he is old enough to be vaccinated. And that’s where we now stand in the year 2017. (Check out the CDC's FAQ on pertussis for a good summary of the issues.) Despite the shortcomings of the current vaccine - it is only around 85% effective and confers immunity for only a few years - no trials of improved vaccines are currently underway. * * * * * * * * * * * * * * * In February of 2005, in anticipation of attending a conference in Eastern Europe, I visited the University of Michigan’s Travel Clinic to make sure my immunizations were up to date and received a routine “tetanus shot.” When I received my paperwork at check-out, I noticed my shot had been recorded as “Tetanus, Diphtheria (age 7-adult) (Td P-Free).” Huh? I’d always thought of the tetanus shot as “DPT.” When I inquired what had happened to the P, I was assured that what I had received was in compliance with CDC recommendations for people over 65. Never mind that I was still three years short of 65; close enough, they said. Then in 2010, a whooping cough epidemic in California made national news, with the highest number of cases reported since 1955, and I once again wondered - not just whether I was adequately protected, but also whether there was any danger of exposing my grandchildren to this disease. I decided I would put the P back in DPT and at my next visit in January 2011 requested the current equivalent recommended for people age 11-64, even though I had now reached the age of 65. Turns out I wasn’t the only one to notice. In October of 2010, the Advisory Committee on Immunization Practices (ACIP) issued a new recommendation that anyone older than 65 be vaccinated for pertussis, though only if s/he had not received a prior dose of Tdap and if s/he expected to have close contact with an infant under one year old. A few months after I made my request, one of the two widely available pertussis vaccines for adults was approved for use in individuals over the age of 65, so an off-label use of the drug was no longer required. Since grandparents have been shown to account for 6-8% of newborn exposure to pertussis, babies were seen as the main beneficiaries of this change, but it also confers an extra measure of protection in seniors whose immune systems might not be working as well as they once did. Still, since immunity wears off after a few years, I couldn’t help wondering why repeat doses still leave out the P. The answer took a little googling but the rationale seems to be twofold: 1) the CDC is investing its efforts in vaccinating pregnant women as its main strategy for protecting infants; and 2) the vaccine has not yet been adequately tested in people over 65. Pharmaceutical companies are apparently compiling data to respond to the second issue as we speak, so watch for a possible change in this policy as well. Even though I don’t currently have a newborn grandchild, I for one am happy to be part of the effort to protect any infant with whom I might come in contact and to contribute to the overall level of herd immunity. I’ve always been a belt-and-suspenders sort of person, so vaccinating pregnant women combined with maintaining high levels of immunity in the general population makes a lot of sense to me. * * * * * * * * * * * * * * * A parting shot for any pregnant woman or mother of a newborn baby: If for whatever reason you've elected not to have yourself or your other children vaccinated - be it mistrust of the government or mistrust of the pharmaceutical industry or religious scruples - or if you haven’t bothered because you’ve never seen a case of whooping cough or think herd immunity will protect your baby, or if you’ve just been too busy to complete your children’s vaccination program, please take a moment to LISTEN TO THESE HEARTBREAKING NARRATIVES shared by women whose lives have been forever changed by pertussis. Losing a child is devastating. Losing a child after knowingly rejecting or neglecting measures that could have prevented that death is beyond devastating. It will haunt you for the rest of your life. Don’t be that mom. Contrary to the belief of many, influenza is not just an especially bad version of a bad cold. It is a highly contagious respiratory disease that strikes suddenly, causing fever, chills, cough, sore throat, runny or stuffy nose, muscle or body aches, headaches, and fatigue. Symptoms can persist for weeks and in some instances lead to hospitalization or death. Children, pregnant women, seniors, young children, and people with certain health conditions are at elevated risk for serious complications. The best prevention is annual flu vaccination. Flu shots are recommended for everyone over age 6 months, except for individuals with allergies to chicken eggs or to certain medications and preservatives, individuals who have experienced a severe reaction to flu vaccination in the past, and individuals who have contracted Guillain-Barré Syndrome within six weeks after a previous flu vaccination. People with a moderate-to-severe illness with a fever should wait until they have recovered. Seniors may not respond adequately to standard dose flu shots and can be given a higher-dose vaccine. On October 7, 2016, The New York Times published an article entitled “Let’s Talk a Millenial Into Getting a Flu Shot.” Why were Millenials singled out? Because a survey of urgent care centers found that more than half of them did not intend to be vaccinated. A 27-year-old Times staff member named Jonah volunteered to offer his own excuses and judge how convincing he found the scientific rebuttals (though as Neil deGrasse Tyson observed, “The great thing about science is that it’s true whether or not you believe it”):
As usual, the very success of flu vaccination, combined with the limited life experience of most young people, has shielded them from the realities of a truly unpleasant flu season. But the particular reluctance of Millenials may also have to do with their being the children of a cohort of parents widely influenced by falsified data linking MMR (measles-mumps-rubella) vaccination to a puzzling apparent increase in autism. This fear, which children born after the mid 1990s imbibed with their mothers' milk, subsequently generalized to all vaccinations and led to widespread distrust of a medical establishment that has overall served us well. In fact, as discussed at greater length in my previous post, there is no scientific evidence whatsoever to support a relationship between vaccination and autism, and the original journal article has long since been debunked and retracted. Nonetheless, just a few weeks ago an article was published in JAMA Pediatrics showing no association of either influenza or influenza vaccination during pregnancy with autism in the child - a line of research that, however reassuring, would probably not be draining resources disproportionately were it not for this cruel hoax. Sadly, these younger Millenials may consequently fail to protect themselves against a number of painful and potentially deadly adult diseases, including pneumonia, shingles, and others to be discussed in a future post. They may also be passing along their own dangerous antiscientific prejudices to the next generation. * * * * * * * * * * * * * * *  As you can guess from my husband’s “flu shot couture,” he and I got our immunizations a couple of months ago, which is when I'd originally planned to post this entry (sigh). Drugstore chains, having discovered that offering immunizations is a good way to lure back-to-school shoppers into their stores, now begin advertising as early as August that supplies of the new vaccine are available. Getting inoculated at the beginning of August is not necessary and may even be a bit too early. Since the vaccine’s protective effects start to taper off within a few months, mid September through early October may actually be the optimal time to be vaccinated and start your "immunity clock" ticking. If you missed that window, however, it's still not too late to get a 2016-2017 flu shot. Immunity following vaccination builds up in about two weeks, and the peak flu season usually runs through January and February. You can be vaccinated at Walgreen’s, Rite Aid, and other major drugstore chains; or you can check online for other options within your community. It’s better to have it right now, even in late December, than to skip it altogether.
Smallpox vaccination, the first successful vaccine in Western medicine’s toolkit, was developed by Dr. Edward Jenner in 1796 after he observed that milkmaids who had caught cowpox, or Variolae vaccinae, a much milder disease, never developed smallpox. Indeed, the term “vaccine” comes from the Latin word for cow. The term vaccine originally referred specifically to smallpox vaccination with the cowpox virus; in 1881 Louis Pasteur, to honor Jenner’s achievement, proposed applying the term generically to all protective inoculations. But before there was Edward Jenner, there was Lady Mary Wortley Montagu. Lady Mary, whose husband served as British ambassador to Constantinople, had occasion while living in Turkey to observe a practice called “variolation.” “Variolation” in some form - involving exposure to a weakened form of smallpox - had long been practiced in parts of China, India, Africa, and the Ottoman Empire, and it was clear to Lady Mary that the procedure was both safe and effective. Having lost a brother to smallpox, which claimed the lives of around 35% of its victims, and having herself been left severely and permanently scarred by the disease, she was prepared to use any means at her disposal to spare her children a similar fate. In 1718 she had her 5-year-old son variolated in Turkey; in 1721, after her return to England, she had her daughter variolated as well during a smallpox outbreak, thus introducing the practice to England. I studied Lady Mary’s writings back in the 1970s, in the course of my research on autobiographies of 17th and 18th century English women. Lady Mary wasn’t a physician or a scientist, nor did she see herself as a medical pioneer. She was simply a devoted mother who used her keen powers of observation and the resources at her disposal to protect her children as best she could. She did exactly what most mothers, guided by the best information available to them, would do in her situation. As a noblewoman, she was also aware that her actions could influence British “fashion” and assumed her example would inspire other mothers to do the same in order to protect their own children - as indeed to some extent it did. (She was far less confident that the medical profession would adopt a practice that would reduce their revenue!) Smallpox vaccination is one of the great successes of modern medicine. In fact, the last endemic case in the world occurred in Somalia in 1977, and no one in the US has been vaccinated since the early 1970s. This is one of the few instances in which not vaccinating is truly safer than vaccinating, since even the rarest or mildest of adverse reactions is unacceptable when the likelihood of anyone’s coming down with smallpox is essentially zero. So far smallpox is the only infectious disease ever to be eradicated. Other candidates such as measles and polio still elude eradication; unfortunately efforts to do so are hampered by campaigns inspired by politics, religion, or anti-science to undermine confidence in vaccination. 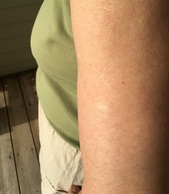 Selfie of my smallpox vaccination scar, almost faded but still visible on my upper arm. You will seldom see this telltale mark on people in their mid forties and under. Once my generation passes they will probably never be seen again. |
Categories
All
Archives
February 2018
|

 RSS Feed
RSS Feed
