|
Poliomyelitis, also known as infantile paralysis or polio, is a highly infectious disease that strikes mainly (but not exclusively) children. It starts innocently enough, like many childhood illnesses, with fever, headache, vomiting, and stiffness or pain. Occasionally, however, the disease invades the central nervous system and causes paralysis, sometimes transient but more often permanent. Thankfully this disease can now be prevented. Consequently, most people in this country have never seen an active case of polio, though many polio survivors born before the mid-1950s remain and indeed have been in the forefront of disability rights advocacy. Isolated cases and localized outbreaks of polio have been described for many centuries, but not until the 20th century did major epidemics begin to occur. The first of these in the US was declared in 1916. Theories, mostly wrong, arose to explain its spread. Dogs and cats were thought to be carriers and tens of thousands of household pets were abandoned or euthanized. Other suspects proposed by the semi-informed or uninformed included mosquitoes, sewers, groundwater, pesticides, flies, bedbugs, subways, and mercury, to name just a few of the more plausible suggestions. As so often occurs, immigrants - at that time mostly Italians - were accused of bringing in and spreading the disease, despite the total lack of evidence of polio in Italy at the time. Children with polio, and even sick children who might or might not have polio, were quarantined in hospitals - many of which barred all visitors, even their parents. The worst outbreak of polio ever seen in America took place in the summer of 1952. Nearly 58,000 cases were reported; of these, 3,145 died and over 20,000 were left with some degree of paralysis. I was nine years old at the time. By then the disease was pretty clearly endemic and people were no longer blaming immigrants, or at least not that I recall. But I remember panicky parents keeping their children away from swimming pools and movie theaters. I remember a neighboring girl - little Linda, barely more than a toddler - wearing metal braces on both legs and walking laboriously with crutches. I remember terrifying photos in the newspaper of children imprisoned in iron lungs for weeks at a time. I also remember the collective sigh of relief breathed by all of America when a successful killed-virus vaccine was approved for use in 1955. Dr. Jonas Salk, the developer, became a national hero overnight. Parents couldn’t get in line fast enough to have their children vaccinated. The advent of the Salk vaccine, and later of an alternative vaccine developed by Dr. Albert Sabin using attenuated live virus, led to the virtual eradication of polio in this country. (There was no cure for polio then; there still isn't. It can only be prevented by vaccination. The last outbreak in the US occurred in 1979, in unvaccinated Amish communities in three states.)
This is the way it’s supposed to be. We should all celebrate wholeheartedly the miracles of modern medicine that have protected us from the ravages of polio and from the whole panoply of diseases that used to kill off more children than survived. We should rejoice that the days in which women carried, gave birth to, and then lost infant after infant, and families had to welcome a dozen or so children just to ensure that a few would live to adulthood, are a thing of the past. Instead, a cruel hoax has resulted in doubt and distrust. Alarmed by an apparent and as yet unexplained increase in autism, anxious parents looked to modern medicine to provide an answer and hoped they’d found one in a paper by Andrew Wakefield, published in 1998 in a prestigious medical journal, The Lancet. Ironically, the article used falsified data to undermine the very medical advances that have done away with three dangerous childhood diseases - measles, mumps, and rubella - by vilifying the MMR vaccine. Like polio, these diseases are usually mild (I suffered through them and so did almost everyone I knew), but a minority of cases result in devastating complications. This paper has since been totally discredited and withdrawn by the editors of The Lancet, but once out of the bottle the genie refuses to go back in. It has turned into a bonanza for Wakefield, who despite having been stripped of his medical license for unethical behavior has achieved celebrity status among parents desperate for some explanation for autism (which coincidentally emerges around the same time as children receive their MMR vaccinations) and continues to profiteer from their misfortune. It has also created a generation of “antivax” parents who distrust not just the MMR vaccine but all vaccines, and indeed, the medical profession and science in general - parents so frightened and suspicious that they are willing to break the social contract whereby we all agree to take a vanishingly small risk to protect the larger community from a much greater danger. A recent NY Times article by Donald G. McNeil Jr. explored the remarkable similarities between the polio outbreak of 1916 and the current outback of another mystifying and terrifying disease, Zika, exactly 100 years later. As McNeil points out, many of the features that characterize our response to Zika, including ugly ethnic prejudice and ineffective measures based on a proliferation of unsubstantiated theories, echo those that emerged in the early days of the polio epidemic. Polio was ultimately banished not by fear-induced lashing out at newcomers and grasping at straws but by the development of an effective vaccine. “All of which may happen with Zika,” says McNeil, “although it can’t happen too soon.” No one could wish for Zika to last a moment longer than necessary. But wouldn't it be remarkable if today’s “antivax” parents, most of whom have themselves been protected by polio vaccination and never experienced anything comparable to what I witnessed as a child, were somehow able to learn from Zika the lessons that the very successes of modern medicine, like the eradication of polio in the US, have enabled many to forget?
0 Comments
Smallpox vaccination, the first successful vaccine in Western medicine’s toolkit, was developed by Dr. Edward Jenner in 1796 after he observed that milkmaids who had caught cowpox, or Variolae vaccinae, a much milder disease, never developed smallpox. Indeed, the term “vaccine” comes from the Latin word for cow. The term vaccine originally referred specifically to smallpox vaccination with the cowpox virus; in 1881 Louis Pasteur, to honor Jenner’s achievement, proposed applying the term generically to all protective inoculations. But before there was Edward Jenner, there was Lady Mary Wortley Montagu. Lady Mary, whose husband served as British ambassador to Constantinople, had occasion while living in Turkey to observe a practice called “variolation.” “Variolation” in some form - involving exposure to a weakened form of smallpox - had long been practiced in parts of China, India, Africa, and the Ottoman Empire, and it was clear to Lady Mary that the procedure was both safe and effective. Having lost a brother to smallpox, which claimed the lives of around 35% of its victims, and having herself been left severely and permanently scarred by the disease, she was prepared to use any means at her disposal to spare her children a similar fate. In 1718 she had her 5-year-old son variolated in Turkey; in 1721, after her return to England, she had her daughter variolated as well during a smallpox outbreak, thus introducing the practice to England. I studied Lady Mary’s writings back in the 1970s, in the course of my research on autobiographies of 17th and 18th century English women. Lady Mary wasn’t a physician or a scientist, nor did she see herself as a medical pioneer. She was simply a devoted mother who used her keen powers of observation and the resources at her disposal to protect her children as best she could. She did exactly what most mothers, guided by the best information available to them, would do in her situation. As a noblewoman, she was also aware that her actions could influence British “fashion” and assumed her example would inspire other mothers to do the same in order to protect their own children - as indeed to some extent it did. (She was far less confident that the medical profession would adopt a practice that would reduce their revenue!) Smallpox vaccination is one of the great successes of modern medicine. In fact, the last endemic case in the world occurred in Somalia in 1977, and no one in the US has been vaccinated since the early 1970s. This is one of the few instances in which not vaccinating is truly safer than vaccinating, since even the rarest or mildest of adverse reactions is unacceptable when the likelihood of anyone’s coming down with smallpox is essentially zero. So far smallpox is the only infectious disease ever to be eradicated. Other candidates such as measles and polio still elude eradication; unfortunately efforts to do so are hampered by campaigns inspired by politics, religion, or anti-science to undermine confidence in vaccination. 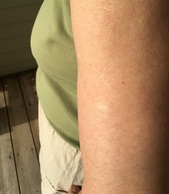 Selfie of my smallpox vaccination scar, almost faded but still visible on my upper arm. You will seldom see this telltale mark on people in their mid forties and under. Once my generation passes they will probably never be seen again. |
Categories
All
Archives
February 2018
|


 RSS Feed
RSS Feed
