 Olivia Twenty Dahl (1955-1962) Olivia Twenty Dahl (1955-1962) In 1962, a seven-year-old girl named Olivia brought home a note from school warning about an outbreak of measles in her class. Soon Olivia too was running a mild fever and covered with red spots. Over the next few days the disease ran its expected course, and her parents weren’t particularly worried. To while away the time, her doting father amused her by telling her stories, teaching her to play chess (at which she promptly beat him), and showing her how to make figures from pipe-cleaners. Then one morning, just as Olivia appeared to be nearly recovered, her father noticed that she had suddenly become feverish and unresponsive, stirring only to moan about a headache. Within just a few hours she was dead from measles encephalitis, a serious complication for which to this day the best medicine can offer is supportive care. Olivia’s father, Roald Dahl, author of such children’s classics as Charlie and the Chocolate Factory and James and the Giant Peach, was “limp with despair.” Dahl was a “do-something” sort of person. When his infant son had suffered brain damage in an accident a couple of years earlier, he had actually set about to design a valve to prevent blockage of the shunt that drained fluid from the brain - and succeeded. He was no biomedical engineer, but when the need arose, he assembled a small team and acquired sufficient expertise to meet the challenge. Now, with Olivia’s life hanging in the balance, there was nothing he could do. He was haunted by his sense of helplessness, compounded after her death by inchoate feelings of guilt that he had somehow let his daughter down. And yet, what could he have done? Twenty-six years later, hoping to extract some shred of meaning from Olivia’s death by sparing others a similar fate, he wrote, “[T]here is today something that parents can do to make sure that this sort of tragedy does not happen to a child of theirs. They can insist that their child is immunised against measles. I was unable to do that for Olivia in 1962 because in those days a reliable measles vaccine had not been discovered. Today a good and safe vaccine is available to every family and all you have to do is to ask your doctor to administer it.” * * * * * * * * * * Measles. The very word sounds slightly risible. Like “Measles the Clown,” perhaps. Or trifling. Like “just some measly childhood disease.” 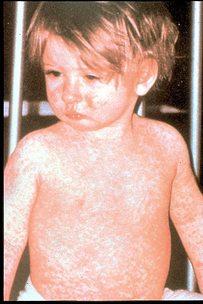 (courtesy of the Centers for Disease Control and Prevention) (courtesy of the Centers for Disease Control and Prevention) But measles is no joke. It is highly contagious and can be spread by an infected person up to four days before before the telltale rash emerges, via tiny airborne droplets produced by sneezing or coughing that remain suspended in the air for two or more hours, even if the infected person is no longer in the room. In many victims the disease runs a benign course, but one in ten are hospitalized, some of whom suffer serious complications including pneumonia and encephalitis. Around 1 or 2 in every 1,000 victims die. Prior to the development of a vaccine, nearly everyone in the US contracted the measles by age 15 - that is, an estimated 3 to 4 million cases/year - so the mortality rate of .1-.2% added up to many thousands of victims per year, mostly children. Measles still causes more vaccine-preventable deaths worldwide than any other infectious disease. A live measles vaccine was first licensed in 1963, just a year after the tragic death of Olivia Dahl, and was superseded by an improved version in 1968. In the twenty years following its introduction in the US, an estimated 52 million cases of measles were prevented, with corresponding dramatic reductions in measles-related complications and death. In the year 2000, measles as an endemic disease was officially “eliminated” from the US; the only reported occurrences of measles were occasional cases introduced from abroad. Truly a public health triumph. Though measles persists globally, most notably in developing countries, aggressive vaccination campaigns have resulted in a precipitous drop in mortality from measles complications worldwide, with a 75% decrease between 2000 and 2013. We now have a measles vaccine that is 97% effective after a single dose and close to 100% effective after a booster dose, which has been recommended since 1985. (Note: People born between 1957 and 1984 should review their immunization status with their doctor, especially if they are planning foreign travel.) To reduce the pain of multiple injections, the vaccine is almost always administered in combination with vaccines for mumps and rubella (MMR) - the first at 12-15 months (earlier if travel abroad is planned), the second at 4-6 years. The rate of serious or life-threatening complications following MMR vaccination is vanishingly small. Although there is NO evidence whatsoever to support a link between MMR vaccine and autism, and although that claim has long since been proved a hoax, the preservative thimerosal (the supposed villain) is no longer used in any vaccine administered to children. As a result, “do-something” parents like Roald Dahl actually have something they can do to ensure that Olivia's fate is not shared by their own child: "They can insist that their child is immunised against measles.” * * * * * * * * * * End of story? Sadly, no. For a disease that’s supposedly been eliminated, measles seems to crop up in the news surprisingly often. After reaching a low of 37 cases in 2004, we now spike record highs every few years, peaking at 667 cases in 2014. A 2013 outbreak occurred at a megachurch in Texas whose pastor had preached from the pulpit against vaccination. In 2015, nearly 200 cases in 24 states were traced to exposure after visits to Disneyland in California. Currently making headlines is an outbreak in Minneapolis, starting in the Somali-American community (fueled by anti-vaccine advocates from outside the community who prey on worries about autism, a malicious genie that refuses to go back in the bottle) and fanning out into the surrounding population through contact in the public schools.
These outbreaks are all shots over the bow. Because international travel is so commonplace, the occasional introduction of measles from abroad is inevitable so long as the disease remains a global scourge. Even more troubling is the occasional case in which no known link to international travel can be found, raising the specter that the disease might once again become endemic. But regardless of the source of any given case of measles, what happens next - whether that single case is self-contained, leads to isolated regional outbreaks, or triggers a full-blown epidemic - depends on how many susceptible individuals are subsequently exposed. Who are these susceptible individuals? As noted above, a handful remain vulnerable even though they have been vaccinated - especially if they have not received a booster dose. In addition, some people are ineligible to be vaccinated because they are very young or very old, because their immune systems are compromised due to illness, because they are pregnant, or in very rare instances because they are allergic to some component of the vaccine. The rest of the susceptible population consists of individuals - mostly children - who though medically eligible have not been vaccinated - and herein lies the problem. Because measles is so highly contagious, vaccination coverage needs to be reach around 95% to maintain “herd immunity” and prevent further spread once a case is introduced. Doing the math, almost everyone who is medically eligible must be vaccinated to prevent the spread of measles, on a regional level or potentially on a much larger scale. Epidemiological studies of measles victims have repeatedly shown that most had not been vaccinated, and of these, the majority had been exempted for non-medical reasons relating religious or philosophical beliefs, or to the systematic spread of discredited data about the health risks of vaccinating (negligible) vs not vaccinating (potentially lethal). Consequently, vaccination rates continue to fall short of the 95% threshold in communities in many areas of the country. The underlying cause of the societal breakdown that could lead to such a situation is difficult to pinpoint. Parents may be uninformed about the importance of completing immunization schedules in a timely manner or persuaded that they cannot trust scientific findings or governmental protections. They may believe their responsibility to their own children takes precedence over the social contract stipulating that we all accept small risks to avoid much larger risks to society as a whole, without understanding the risks to which they subject their own children by leaving them defenseless against measles. Government agencies in turn may succumb to pressure to issue non-medical "personal belief" exemptions or be reluctant to enforce existing vaccination requirements. People with far more expertise than I can claim have yet to figure out where to intervene in this chain and how hearts and minds can be changed. Part of the problem, of course, is that thanks to the very success of immunization campaigns, many Americans have lived their entire lives without having witnessed the ravages of a major epidemic. Let us hope an answer can be found that doesn't require a reintroduction of some of the terrifying communicable diseases medical science has conquered. How fortunate we are to live in a time and place where children like Olivia no longer need to die as their parents stand by helplessly. How sad that some will anyway, and that there is no immediate end in sight to this trend.
0 Comments
Poliomyelitis, also known as infantile paralysis or polio, is a highly infectious disease that strikes mainly (but not exclusively) children. It starts innocently enough, like many childhood illnesses, with fever, headache, vomiting, and stiffness or pain. Occasionally, however, the disease invades the central nervous system and causes paralysis, sometimes transient but more often permanent. Thankfully this disease can now be prevented. Consequently, most people in this country have never seen an active case of polio, though many polio survivors born before the mid-1950s remain and indeed have been in the forefront of disability rights advocacy. Isolated cases and localized outbreaks of polio have been described for many centuries, but not until the 20th century did major epidemics begin to occur. The first of these in the US was declared in 1916. Theories, mostly wrong, arose to explain its spread. Dogs and cats were thought to be carriers and tens of thousands of household pets were abandoned or euthanized. Other suspects proposed by the semi-informed or uninformed included mosquitoes, sewers, groundwater, pesticides, flies, bedbugs, subways, and mercury, to name just a few of the more plausible suggestions. As so often occurs, immigrants - at that time mostly Italians - were accused of bringing in and spreading the disease, despite the total lack of evidence of polio in Italy at the time. Children with polio, and even sick children who might or might not have polio, were quarantined in hospitals - many of which barred all visitors, even their parents. The worst outbreak of polio ever seen in America took place in the summer of 1952. Nearly 58,000 cases were reported; of these, 3,145 died and over 20,000 were left with some degree of paralysis. I was nine years old at the time. By then the disease was pretty clearly endemic and people were no longer blaming immigrants, or at least not that I recall. But I remember panicky parents keeping their children away from swimming pools and movie theaters. I remember a neighboring girl - little Linda, barely more than a toddler - wearing metal braces on both legs and walking laboriously with crutches. I remember terrifying photos in the newspaper of children imprisoned in iron lungs for weeks at a time. I also remember the collective sigh of relief breathed by all of America when a successful killed-virus vaccine was approved for use in 1955. Dr. Jonas Salk, the developer, became a national hero overnight. Parents couldn’t get in line fast enough to have their children vaccinated. The advent of the Salk vaccine, and later of an alternative vaccine developed by Dr. Albert Sabin using attenuated live virus, led to the virtual eradication of polio in this country. (There was no cure for polio then; there still isn't. It can only be prevented by vaccination. The last outbreak in the US occurred in 1979, in unvaccinated Amish communities in three states.)
This is the way it’s supposed to be. We should all celebrate wholeheartedly the miracles of modern medicine that have protected us from the ravages of polio and from the whole panoply of diseases that used to kill off more children than survived. We should rejoice that the days in which women carried, gave birth to, and then lost infant after infant, and families had to welcome a dozen or so children just to ensure that a few would live to adulthood, are a thing of the past. Instead, a cruel hoax has resulted in doubt and distrust. Alarmed by an apparent and as yet unexplained increase in autism, anxious parents looked to modern medicine to provide an answer and hoped they’d found one in a paper by Andrew Wakefield, published in 1998 in a prestigious medical journal, The Lancet. Ironically, the article used falsified data to undermine the very medical advances that have done away with three dangerous childhood diseases - measles, mumps, and rubella - by vilifying the MMR vaccine. Like polio, these diseases are usually mild (I suffered through them and so did almost everyone I knew), but a minority of cases result in devastating complications. This paper has since been totally discredited and withdrawn by the editors of The Lancet, but once out of the bottle the genie refuses to go back in. It has turned into a bonanza for Wakefield, who despite having been stripped of his medical license for unethical behavior has achieved celebrity status among parents desperate for some explanation for autism (which coincidentally emerges around the same time as children receive their MMR vaccinations) and continues to profiteer from their misfortune. It has also created a generation of “antivax” parents who distrust not just the MMR vaccine but all vaccines, and indeed, the medical profession and science in general - parents so frightened and suspicious that they are willing to break the social contract whereby we all agree to take a vanishingly small risk to protect the larger community from a much greater danger. A recent NY Times article by Donald G. McNeil Jr. explored the remarkable similarities between the polio outbreak of 1916 and the current outback of another mystifying and terrifying disease, Zika, exactly 100 years later. As McNeil points out, many of the features that characterize our response to Zika, including ugly ethnic prejudice and ineffective measures based on a proliferation of unsubstantiated theories, echo those that emerged in the early days of the polio epidemic. Polio was ultimately banished not by fear-induced lashing out at newcomers and grasping at straws but by the development of an effective vaccine. “All of which may happen with Zika,” says McNeil, “although it can’t happen too soon.” No one could wish for Zika to last a moment longer than necessary. But wouldn't it be remarkable if today’s “antivax” parents, most of whom have themselves been protected by polio vaccination and never experienced anything comparable to what I witnessed as a child, were somehow able to learn from Zika the lessons that the very successes of modern medicine, like the eradication of polio in the US, have enabled many to forget? |
Categories
All
Archives
February 2018
|

 RSS Feed
RSS Feed
